Clinical Features
Co-infection
Co-infection occurs when a person becomes infected simultaneously with HBV and HDV. The most common outcome is complete recovery and clearance of both viruses. In less than 5% of cases, patients develop chronic infections. In about 1% of cases, infection results in fulminant hepatitis.
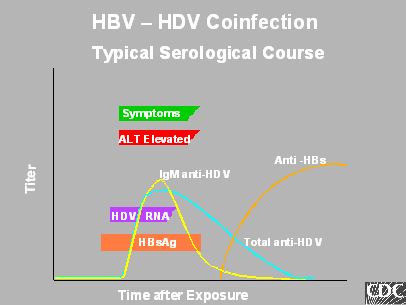
http://www.cdc.gov/ncidod/diseases/hepatitis/slideset/hep_d/slide_4.htm
Super-infection
Super-infection occurs when a person who is already seropositive for HBV becomes infected with HDV. It is associated with more severe clinical outcomes than co-infection with HDV. Fulminant hepatitis develops in about 5% of cases. 80-90% of infections will become chronic, increasing the rate with which patients develop cirrhosis. The chance of developing hepatocellular carcinoma (liver cancer) also increases.
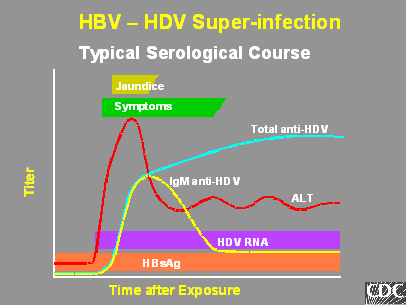
http://www.cdc.gov/ncidod/diseases/hepatitis/slideset/hep_d/slide_5.htm
Symptoms
As many as 90% of infected patients may be asymptomatic. Common symptoms are jaundice, dark urine, abdominal pain, fever, and nausea with emesis. Confusion, bruising, bleeding, and encephalopathy are rare.
Differential Diagnosis
HDV infection can be difficult to distinguish from other causes of hepatitis. The differential diagnosis includes other viruses, other infectious causes, and some non-infectious causes.
Viruses:
|
Hepatitis A |
|
Hepatitis B |
|
Hepatitis C |
|
Hepatitis E |
|
Cytomegalovirus |
|
Yellow fever |
|
Ebola |
|
Marburg |
Infectious Causes:
|
Amebiasis |
|
Fasciola |
|
Liver flukes |
Non-infectious Causes:
|
Alcoholic hepatitis |
|
Liver abcess |
|
Biliary obstruction |
|
Mushroom toxicity |
|
Acetominophen poisoning |
|
Drug-induced hepatitis |
Laboratory Tests
--Serologic assays for HDV-RNA and δAg
--Antibody assays for anti-HDV IgM and IgG
--Imaging of upper right quadrant to check for biliary obstruction and hepatocellular carcinoma
--Immunohistochemical analysis of liver tissue in causes of suspected persistant HDV infection
Treatment
There is currently no vaccine or immune globulin available
for HDV. Antiviral treatment consists of
interferon alpha. Antivirals such as
lamivudine and ribavirin, which work against other forms of viral hepatitis,
appear to be ineffective in treating HDV infection.